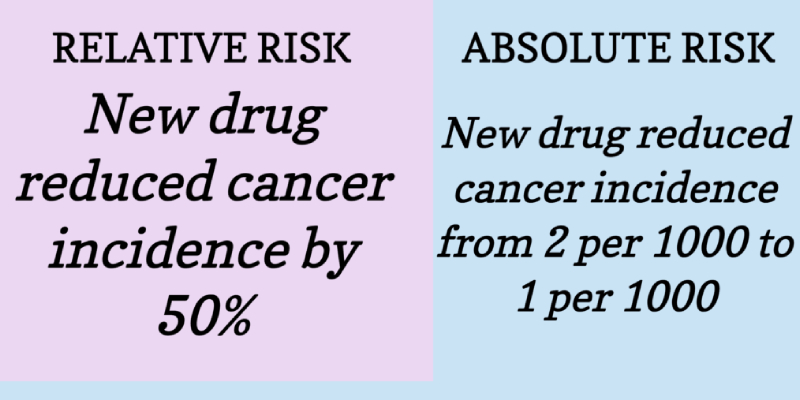Given the unbearable costs hospital errors exact on our nation’s sick and injured population every year, it’s sometimes hard to muster optimism. However, a December 2014 report published by the Department of Health and Human Services suggests that medical workers and hospital safety experts may finally be winning the battle – or at least turning the tide.
- The report said that “hospital acquired conditions” (e.g. staph infections caught in a hospital ER) declined over a three year period by 17 percent.
- Medical errors, meanwhile, declined in practically every category.
- IV blood infections, for instance, declined by almost 50 percent.
- Bedsore ulcers — a plague that visits bedridden patients who are not moved frequently enough — declined by 20 percent.
- Pharmaceutical errors also declined by nearly 20 percent.
The timeframe of the report covers 2010 to 2013.
In 1999, the Institute of Medicine found that such errors killed approximately 98,000 people a year in the United States. Later analysis determined that number could be much higher.
Some analysts credit the decrease in errors to the Affordable Care Act (a.k.a. “Obamacare”), which incentivizes hospitals through the “Partnership for Patients” program. This policy has been associated with a reduction in re-admissions (by 18 percent as of early 2014). A pilot program run at Mount Sinai Hospital in New York City found that a similar incentive system led to a drastic cut in re-admissions by over 40 percent.
However, an analysis published in 2012 in the New England Journal of Medicine suggested that government incentives do not necessarily correlate with decline in certain hospital infections.
Hopefully, researchers will analyze this progress more carefully and help us uncover how to make hospitals safer and less error-prone.